Cancer is one of the most emblematic diseases of aging in developed countries. As life expectancy has increased considerably over the past century, it has become one of the leading causes of death today. Indeed, its incidence is now high (nearly 400,000 new cases diagnosed in France in 2017) and mainly affects the elderly (median age at diagnosis: 67 years)[1].
Cancer as a disease of aging: what is it, exactly?
The purpose of this article is to explain as fully as possible how cancer works. We will see that the cancerous tumour is a much more complex element than the simple cluster of aberrant cells responsible for the dysfunction of our body. In their journal Hallmarks of Cancer: The Next Generation[2], Drs. Hanahan and Weinberg describe the top 10 hallmarks of cancer.
- Sustaining proliferative signaling for cancer cells
- Evading growth suppressors
- Resisting cell death
- Enabling replicative immortality
- Inducing angiogenesis (producing new blood vessels)
- Activating invasion and metastasis
- Genome instability and mutations
- Tumor-promoting inflammation
- Deregulating cellular energetics
- Avoiding immune destruction
We will detail each of these points here and use them to understand why cancer is an age-related disease.
1) Cancer wants to maintain signals to proliferate at all costs

One of the main and most well-known aspects of malignant tumours is that they are composed of cells that proliferate chronically, apparently uncontrollably. Indeed, in normal, healthy tissue, cell division is extremely regulated. This only occurs when growth factors are released to maintain the function of a given tissue. The tumor is characterized by a constant activation of these proliferation signals on which it depends to grow.
To escape from this control system, the tumor has several means. The first, and most obvious, is to produce its own growth factors[3]! Even more surprisingly, it can even force the surrounding healthy tissues to produce it for itself while growing at its expense, as a parasite would do[4]. The proliferation control system is then defeated by its own rules.
One of the main characteristics of cancer cells is their high number of genomic mutations and modifications. They may also be responsible for cancer cells escaping any control and proliferating. By accumulating mutations on specific genes, either to activate proliferation in the event of growth factor reception[5] or to prevent it in its absence[6], the tumour can continue to grow permanently. Like a switch locked in ON mode, it becomes free of any form of external control.
2) Cancer wants to ignore all the warning messages that could hinder its growth
When there is a problem, the body can send many signals to prevent growth until the situation improves. Nevertheless, the tumor learns to ignore them. Let’s see how.
First, the cancer cell learns not to “listen” to its warning proteins. The two main alert proteins are RB and p53. As the tumor grows, it greatly affects its environment, and RB serves as an integrator for this information[7]. p53 is used to measure the damage that accumulates inside the cell, which is then high in the case of uncontrolled proliferation. These two proteins are among the most frequently mutated in cancer, allowing associated tumours to grow at any cost[2]. Other systems exist to prevent a tissue from growing, especially if it invades the space of its neighbours. Many surface proteins allow cells to adhere to each other. They thus form a kind of “molecular velcro” that will recruit other proteins that will, in turn, send a signal preventing cells from dividing, to avoid overpopulation in a space that can not accommodate more cells. Cancer cells have the ability to completely ignore these signals and continue to proliferate despite the lack of space[8].

However, the body has another tool to block growth if it needs to. A class of signalling molecules, TGF-β, is secreted by surrounding tissues to stop growth. Again, the tumour learns to turn a deaf ear. Worse, it can reshape the effects that TGF-β has on it[9]. Not only do they not prevent it from growing, but they also help it to achieve a key stage in its evolution that we will see later: metastasis.
3) Cancer wants to create artificial immortality to resist cell death
Not only do cancer cells proliferate without restriction, they are also very hard to destroy. They are indeed made much less sensitive to the phenomenon of classical cell death: apoptosis[10].

We have previously discussed the role of the p53 protein in stopping proliferation in case of internal damage. However, if the damage is too severe, p53 is then one of the main mediators of apoptosis, the process of cellular suicide. Because tumor cells are very active, they are subjected to many sources of cellular stress leading to the accumulation of damage. Unlike healthy cells, however, they will be much less sensitive to the mechanisms used by p53 to induce their suicide, becoming virtually “immortal”[11].However, a cancer cell is no more resistant to damage than any other, it just seems to be unaware of it. By allowing damage to accumulate in this way, the cell eventually malfunctions completely. It then ends up dying “involuntarily”: this is called necrosis. Unfortunately, this phenomenon has a sad consequence: the release of growth factors. Thus, if by accident a cancerous cell dies, it stimulates its neighbours to proliferate even more[12]!
4) Cancer wants to be able to proliferate indefinitely
We explained it in our articles on telomeres and aging: when a cell divides, the ends of its chromosomes (called telomeres) shrink. When the telomeres are completely destroyed, the cells normally enter apoptosis or senescence (they stop dividing)[2]. Under normal conditions, it is therefore impossible to proliferate indefinitely. So how do tumors do it?
To prevent telomeres from shrinking, tumor cells use an enzyme called telomerase. It is normally only expressed in our stem cells in adulthood. It allows telomeres to regenerate between cell divisions. In this way, stem cells can play their essential role throughout our lives. In the hands of cancer, this life-saving tool turns against us and allows cancer cells to replicate infinitely[13]. Moreover, it would seem that telomerase does not only have this repair role, it would also amplify the growth signals, thus allowing the tumor to grow even faster[14]!
Nevertheless, it has been shown that the absence of telomeres can also promote cancer. It is possible that two chromosomes without telomeres may merge. These chromosome “patchworks” can have an effect similar to certain mutations and promote tumor growth[15]. Thus, with or without telomerase, the tumor adapts.


5) The cancer wants supply from many blood vessels
Like any type of tissue, to grow and survive, the tumour needs to be supplied with oxygen and nutrients[16]. To do this, cancer cells need blood vessels that can supply them. To this end, they will secrete a growth factor called VEGF, which functions as a vascular cell magnet and will encourage the formation of new vessels[17]. This process is called angiogenesis.
It has been shown that this formation of vessels, called neovascularization, occurs very early in the formation of the tumor. In addition to certain proliferation pathways that promote VEGF synthesis, some cancer cells will become hypoxic because they do not receive enough oxygen. The normal response to hypoxia includes a significant secretion of VEGF[18]. Thus, as soon as it forms, the tumour has all the tools it needs to acquire an important supply of nutrients thanks to the secretion of VEGF and the formation of new vessels, whose growth is sometimes anarchic[19].
6) Metastasis: cancer invades the rest of the body
The aspects we have seen so far describe the formation and growth of a tumour in a given location. Unfortunately, the tumour can, through the metastasis process, invade the rest of the body. We have seen earlier that cells in a tissue are anchored through a ” molecular velcro ” to their environment. Cancer cells are no exception. In addition, a separation of this velcro normally results in a particular form of apoptosis called anoïkis[20]. Moreover, tumor cells are not programmed to move inside the tumor. So how do they manage to free themselves from all these constraints to invade our body?

Departure day
After many years of research, the scientific community has identified the majority process behind this migration, “Epithelial-Mesenchymal Transition” (EMT), reflecting the transition from a fixed cell state (called epithelial) to a mobile (mesenchymal type). This process is normally observed during our embryonic development[21] or during wound healing[22]. In these two physiological cases, this process allows a set of cells to migrate to other tissues to ensure their function. This process includes two main steps. The first is losing the neighbouring cells that allow it to stick to its external environment. It’s the Velcro detachment. This is combined with a repression of the mechanisms that should have resulted in cell death by anoïkis. The second is the acquisition of what is called the migratory phenotype. The cell becomes able to digest or migrate the proteins surrounding it. This allows it to move as it pleases[23]. It is therefore by appropriating this physiological process that cancer cells become able to leave the tumour..
One could think that this phenomenon of the tumour’s departure is more a matter of chance, that it would be due to a random reprogramming of cancer cells. It has been shown that in response to molecules secreted by the tumor, healthy mesenchymal cells[24] or macrophages (cells of our immune system)[25] could induce cancer cells to perform EMT. These macrophages could also facilitate the formation of metastases by digesting the environment around the tumor. This would allow cancer cells to leave it easily[26].
A complicated settlement
Once the cancer cell leaves the tumor, it tries to settle somewhere else. But things are not that easy. Indeed, we generally observe myriads of disseminated micro-metastases that never succeed in re-forming tumors[27]. The commonly accepted reason for this is that the metastatic cancer cell is not adapted to the environment it colonizes. It may not have a way to form new blood vessels[28]. It can also suffer from a severe lack of nutrients or lack of growth factors[29]. These two deficiencies lead to the metastasis becoming dormant, preventing it from forming a new tumor. Some studies suggest that tumors from certain tissues can only produce metastases adapted to other specific tissues[27]. It would be necessary for the environment colonized by metastasis to be perfectly adapted. When this happens, the consequences are severe for the patient, in whom tumors can multiply.

7) Cancer destabilizes its genome to better adapt

The first 6 characteristics we have just mentioned require a different use of many proteins, or even their modification. To achieve this, the cancer cell must make significant changes within its genome. This can happen through the methylation of its DNA [30]. However, it is not these epigenetic modifications that would have the most important role.
Indeed, the cells have found the solution to evolve and adapt more quickly: drastically increase the appearance of mutations in our genome[31]. The central protein in genome monitoring, as already mentioned, is p53[32]. Its inactivation with that of proteins to detect, repair or protect the genome is found in most tumours[31]. These inactivations are the main hypothesis to explain the ability of cancer to transform and adapt to form tumors as we know them.
8) Cancer uses inflammation to its advantage
Contrary to what one might think, the inflammatory environment favors cancer cells in many ways because it is full of growth factors that promote their proliferation and adaptation (such as VEGF) as well as survival factors that prevent them from entering apoptosis. Immune cells also release molecules capable of promoting the appearance of metastases, but also molecules capable of increasing the mutation rate of cancer cells[12 & 33].
Thus, inflammation, despite its intended role as an anti-tumor protection, ultimately acts as a catalyst by promoting its expansion.

9) Cancer adapts its metabolism to the challenges of its environment
Cancer needs a lot of energy to grow. This is one of the reasons why he develops such an important vascularization. However, it is far from perfect. As a result, a large proportion of the cancer cells in the core of the tumour have very little oxygen, which is essential for the functioning of their mitochondria. These organelles are able to produce large quantities of ATP, the fuel for our cells via a process that some of the tumor cells cannot accomplish due to a lack of oxygen.

However, once again, cancer adapts. The solution? Absorb much more glucose than normal cells. The cancer cells then simply degrade it into pyruvate, a process that does not require oxygen, but 18 times less efficient than if the mitochondria were functional[34]. This process is all the more facilitated because it involves the genetic pathways involved in the reception of growth factors or even lack of oxygen[35 & 36].
Even more interesting, it would seem that a form of organization of energy resources and communication exists between cancer cells that do not have access to oxygen and their better supplied neighbours. The non-oxygenated cells would transform the pyruvate they produce into lactate, before releasing it into the intercellular medium. This would then be captured by cells with available oxygen. The lactate would then serve as fuel for their mitochondria, which have the necessary oxygen at their disposal[37]. Zero waste!
10) Cancer learns to hide from the immune system
The immune system is the main enemy of cancer inside the body. Indeed, in patients with tumors highly infiltrated by lymphocytes, the survival rate is much higher, indicating the major role of our immune system[38]. Tumor cells must therefore learn to defend themselves against it and to avoid it. We will list the different ways in which tumors protect themselves from the immune system in our last section on the main progress made in the fight against cancer in recent years: immunotherapy.

Cancer and aging
Now that we have a clear idea of what a cancerous tumour is and how it works, a question arises: why does it affect us especially when we get older? Most of the characteristics of cancer require alteration of the genome of its cells. However, the alteration of the organization of the genome is one of the characteristic factors of aging. By accumulating, over time, alterations in our genome, we provide fertile ground for tumors to appear[39].

Another probable reason for the emergence of cancers with age would also be the decrease in the effectiveness of the immune system. With age, the immune system ages as well and no longer achieves the performance it could have before. Cancer could thus proliferate without any obstacle, leading to an increase in the number of tumours observed in the elderly[40].
However, it should be noted that none of these hypotheses has so far been clearly proven. Indeed, some are even contested. For example, it has been shown that a large number of cells that have accumulated mutations in the elderly, which are supposed to promote tumor development, do not do so[41]. The same researchers also argue that the period when the cells in our body accumulate the maximum number of mutations is during its development. Thus, cancers should occur much earlier if the simple accumulation of mutations was responsible for the formation of cancers.
Overcoming cancer in aging: a challenge soon to be mastered?
When the body can no longer contain the tumor, cancer cells invade it until it causes its general dysfunction. That is why researchers and doctors have been working for decades to find a cure for this disease.
Traditional anti-cancer therapies:
The two most common treatments, and most often combined to treat cancer, are chemotherapy and radiotherapy. Chemotherapy is, as its name suggests, a treatment based on chemical molecules. These aim to damage rapidly dividing cells by interfering with different stages of the cell cycle (stages that the cell goes through when it divides)[42]. As cancer cells proliferate abundantly, they are particularly affected. Unfortunately, in our bodies, many cells must also divide. Chemotherapy does not sort out which ones it kills. Thus, chemotherapy causes strong side effects. These include hair loss, a sharp decrease in the number of blood cells and a dysfunction of the digestive system[43].

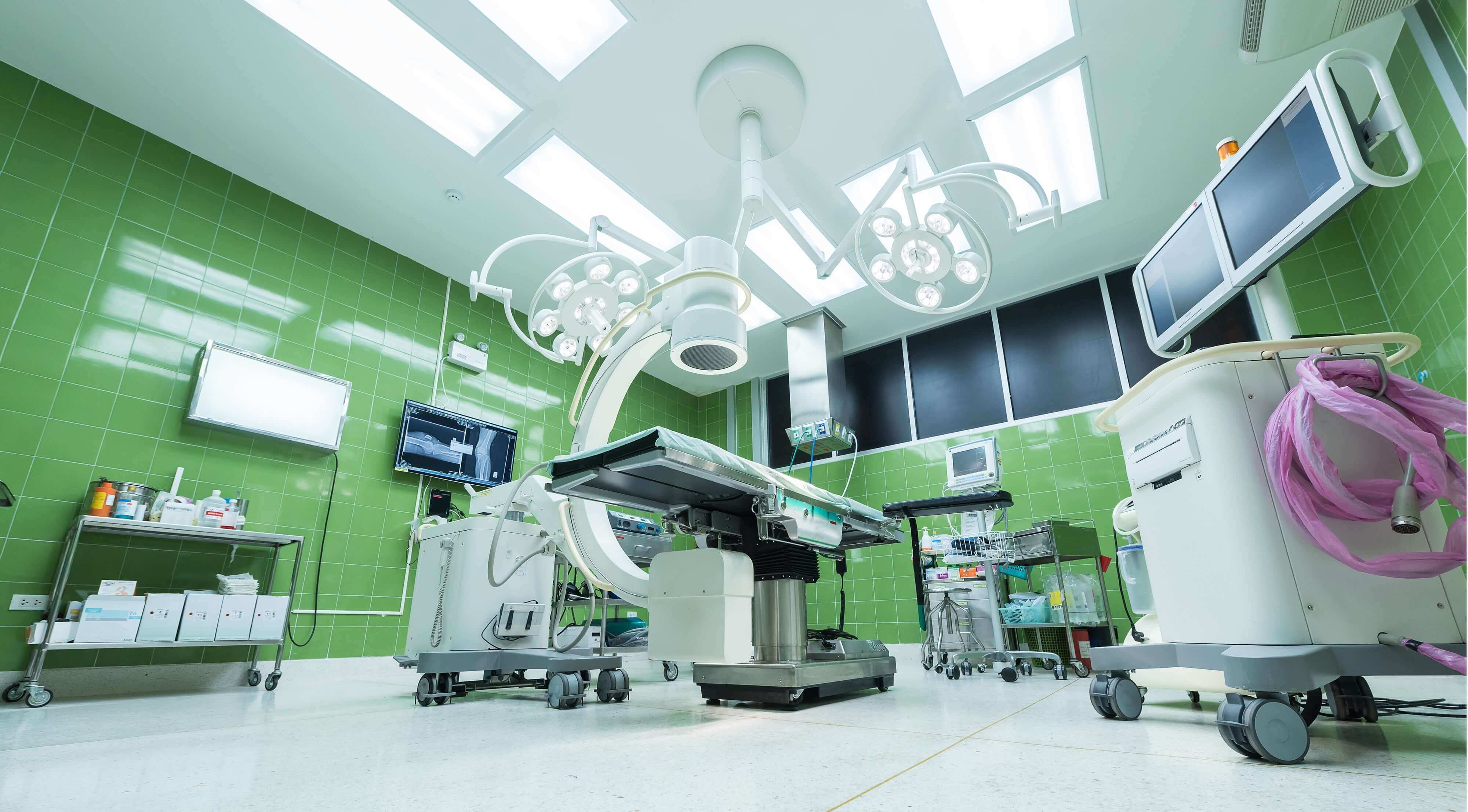
Radiotherapy is a more targeted approach. This technique is based on the use of X-rays directed against the tumor. These rays cause the appearance of charged, high-energy molecules that damage the DNA of the target cells[44]. Normal cells have many mechanisms for repairing their DNA, so they are able to survive. However, cancer cells, as we have seen, have deficient DNA repair systems, so they are not X-ray resistant[45]. However, radiotherapy alone contributes on average only 40% to the total removal of the tumor[46], so it is necessary to combine it with other treatments, such as chemotherapy or surgery.
The use of these techniques should, in theory, allow to eliminate all tumour cells. So how to explain the number of relapses after these treatments?
Cancer stem cells: the new target to tackle
Stem cells are the cells that create all the cells in our organs. Although not directly involved in their function and very few in number, their role is crucial. Located in a subpart of the organ called a niche, they are the ones who have the capacity to recreate new cells, to renew them regularly. Without these, the tissues become damaged and cannot be repaired. What if cancers work the same way? This would explain the phenomena of tumour relapse after treatment, tumour dormancy and metastasis observed[47].
What is a cancer stem cell?
The idea that cancers are also based on a stem cell system comes from tumor transplant experiments. For example, it has been shown that only a subset of cancer cells in leukemia, breast, brain and many other organs, can recreate a new tumour if transplanted alone[47]. This suggests that, as with normal organs, only some specific cells can fully recreate it: stem cells. Could this not be the explanation for the failure to implant the majority of metastases, only cancer stem cells (largely in the minority), with the ability to form new tumours? Could they be the cells that cause relapses after the apparent disappearance of tumours after treatment?

Cancer stem cells and therapies: new challenges
Why do cancer stem cells resist chemotherapy and radiation therapy? The reason would be precisely their stem cell properties. Stem cells have more means to protect their genome, are less likely to divide and may even enter a state of quiescence[48]. Chemotherapy and radiotherapy are therefore unnecessary against them. After treatment, cancer stem cells survive as much as surrounding cells and only have to form new tumors again.

So how do we fight this type of cell? The first technique is to use drugs that prevent them from remaining stem cells, forcing them to become normal cancer cells. Encouraging results have been obtained with this technique to treat leukemias[49] or colorectal cancer[50]. The other method is to target their environment. To remain a stem cell, a cell must constantly receive signals from its surroundings: its niche. By interfering with these signals, several studies have shown promising results and two clinical trials have been launched to treat pancreatic, lung and breast cancers[48].
Thus, if these approaches prove to be successful, we would have all the tools at our disposal to permanently eliminate tumors.
Immunotherapy and cancer: provide our body with more effective weapons
The immune system actively fights the tumor in formation, but often finds itself overwhelmed. Research has developed immunotherapies by studying cancer’s escape mechanisms.
Antibodies to preserve the immune system
To resist our immune system, cancer cells can try to “convince” it not to attack them. For example, a cancer cell can use a protein normally expressed at the end of inflammation by healthy cells: PD-L1[51]. When immune cells, especially lymphocytes, are exposed to PD-L1 protein, they do what they are supposed to do once the danger is eliminated: they die[52]. Researchers have chosen to consider how to physically block this mechanism by using antibodies that bind to PD-L1 or PD-1 (the PD-L1 receptor, expressed by lymphocytes). Clinical trials have proven the effectiveness of these antibodies as anti-cancer treatment and they are now used to treat many cancers[51].
However, sometimes allowing our lymphocytes to survive is not enough, we must also find a way to make them more aggressive against cancer. One of the causes of this lack of aggressiveness is the CTLA-4 protein, expressed by the lymphocytes themselves. It normally prevents over-inflammation, which could escalate. However, in the fight against cancer, boosting lymphocytes can be beneficial. Thus, the same blocking technique is used for CTLA-4 as for PD-L1 and PD-1. This technique, like the previous one, has proven effective in the fight against certain types of cancer and is now used as a treatment in hospitals[53].
However, when playing with fire it is possible to burn oneself. If these mechanisms for regulating our immunity exist, it is to prevent it from attacking our own bodies and destroying them. Thus these techniques, although effective against cancer, can have important side effects. It is therefore sometimes necessary to take heavy anti-inflammatory treatment after these to prevent the situation from escalating[54].
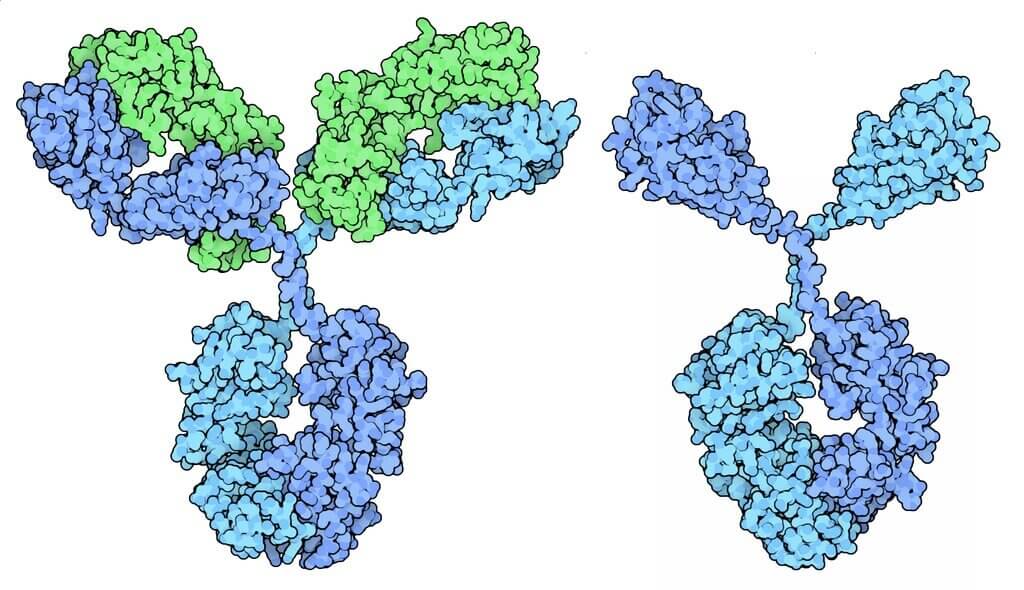
Why not develop an anti-cancer vaccine?
As with other diseases, our immune system must recognize cancer as a threat before attacking it. The principle of vaccination is to make our immune system understand that we must fight a specific disease and this principle is now being developed to fight cancer[55]. To do this, we must find the right method to stimulate our immunity only against the tumor. Let’s look at four approaches that are currently being studied.
For our lymphocytes to recognize a danger, another type of cell called antigen presenting cells (APCs) must alert them to it. Normally, the lymphocytes that can recognize cancer are not active. The CPA must show them the cancer protein they can recognize so that they can proliferate and move to the tumor site to eradicate it. This is the mechanism used by the first type of vaccine[55]. By injecting the patient with a mixture of proteins expressed by cancer cells and molecules that attract CPAs, they will effectively stimulate lymphocytes. This technique, directly inspired by conventional vaccination techniques, has already proven its effectiveness against cancer in clinical trials[56].
The second technique is similar to the cellular therapy that we will describe later. It consists of extracting the patient’s CPAs and bringing them into contact with proteins from cancer cells in vitro. Once they have absorbed these proteins, they are re-injected into the patient’s body to activate the lymphocytes against cancer[57]. Many clinical trials are also underway for this treatment[58].
The third vaccine technique is even more inventive, taking cells from the patient’s cancer and genetically modifying them to attract CPAs. Once re-injected, they are destroyed by the CPAs, which will be able to activate anti-cancer lymphocytes[55]. Again, this treatment is currently in clinical trials[59].
The last technique we describe is at the crossroads between gene therapy and a vaccine. By using viruses that express on the surface of cells that they infect pieces of protein expressed by tumours, they stimulate the immune system of patients against cancer. Indeed, the immune system is much better at recognizing cells infected with viruses than cancer cells. The cells infected with the virus will therefore be quickly destroyed by the patient’s CPAs, which will then be able to supply cancer proteins to the lymphocytes[55]. Once again, these treatments are still in clinical trials[60].
Act directly on lymphocytes through cell therapy
The vaccine techniques we have described are used to stimulate anti-cancer lymphocytes indirectly, through CPAs. Nevertheless, other techniques exist to act directly on these lymphocytes. We will discuss here the two most common and promising methods.

The first method we will describe exploits the fact that even if cancer actively represses lymphocyte activity, it cannot do so completely. Thus, it is possible to find lymphocytes inside tumors that are trying to destroy them: “Tumor Associated Lymphocytes” (TIL). Since these TILs are already naturally directed against the tumor, why not use them? The principle is as follows: TILs are extracted from the tumor and then forced to proliferate in vitro. After testing their ability to destroy cancer cells, the most effective ones are then injected back into the patient’s body in large numbers[61]. Thus, the patient is equipped with a large number of lymphocytes already activated and very effective to fight against the tumor. Today, several companies now offer this type of therapy to fight cancer[62].
Unfortunately, cancer has another weapon to fight lymphocytes. For a lymphocyte to be able to inspect a cell, it must show it pieces of its own proteins. These pieces of protein, called antigens, are presented to the lymphocyte on a protein called MHC (Major Histocompatibility Complex). Without it, the lymphocyte cannot act. Cancer cells use this bias to escape lymphocytes: they simply stop showing their antigens on the MHC. Thus, even if very many TIL are present, the tumor cannot be destroyed[63]. How to solve this major problem? The solution lies in the use of genetic engineering. Researchers have found a way to recreate a lymphocyte receptor from scratch that can recognize the tumor without expressing MHC. The patient’s lymphocytes are collected and then genetically modified to express this artificial receptor: we speak of CAR-T cells[64]. Once re-injected into the patient, these cells can then destroy the tumor. This very promising therapy method was tested at the beginning of 2018 in more than 250 clinical trials[64] but still has some flaws. The main side effect would be the direct consequence of too high an efficacy of these lymphocytes, which no longer require MHC to activate. The inflammation they cause would then be so strong that the blood-brain barrier protecting the brain from the blood system would become weakened by pro-inflammatory molecules. Patients treated with CAR cells may then suffer from multiple small brain haemorrhages with a highly neurotoxic effect[65].

As we have just seen, tremendous progress has been made in recent years in understanding the formation and growth of cancer. This knowledge is now giving rise to new and increasingly sophisticated treatments to fight tumours. Although these advances are currently facing many side effects and need improvement, they are more than promising. Could cancer no longer be a deadly phenomenon in the near future? The future will tell.
Diseases of aging: our articles
Baptiste Tesson

Author
Auteur
Baptiste is studying biology at the École Normale Supérieure de Lyon and bioengineering at the École Polytechnique Fédérale de Lausanne. He worked on the optimization of Cas9 as a tool for genome editing and on the emergence of blood stem cells in the zebrafish. He currently works on the patterning of the muscles, also in the zebrafish. He plans on doing a PhD in developmental biology.
More about the Long Long Life team
Baptiste étudie la biologie à l’École Normale Supérieure de Lyon et la bioingénierie à l’École Polytechnique Fédérale de Lausanne. Il a travaillé sur l’optimisation de la protéine Cas9 comme outil de modification de génomes et sur le développement des cellules souches du sang chez le poisson zèbre et travaille actuellement sur la mise en place des muscles chez le même animal. Il projette de réaliser un doctorat axé vers le développement animal.
En savoir plus sur l’équipe de Long Long Life
References:
[1] http://www.e-cancer.fr/Professionnels-de-sante/Les-chiffres-du-cancer-en-France/Epidemiologie-des-cancers/Donnees-globales
[2] Hanahan, D., & Weinberg, R. A. (2011). Hallmarks of cancer: the next generation. cell, 144(5), 646-674.
[3] Witsch, E., Sela, M., and Yarden, Y. (2010). Roles for growth factors in cancer progression. Physiology (Bethesda) 25, 85–101.
[4] Cheng, N., Chytil, A., Shyr, Y., Joly, A., and Moses, H.L. (2008). Transforming growth factor-beta signaling-deficient fibroblasts enhance hepatocyte growth factor signaling in mammary carcinoma cells to promote scattering and invasion. Mol. Cancer Res. 6, 1521–1533.
[5] Davies, M.A., and Samuels, Y. (2010). Analysis of the genome to personalize therapy for melanoma. Oncogene 29, 5545–5555.
[6] Wertz, I.E., and Dixit, V.M. (2010). Regulation of death receptor signaling by the ubiquitin system. Cell Death Differ. 17, 14–24.
[7] Burkhart, D.L., and Sage, J. (2008). Cellular mechanisms of tumour suppression by the retinoblastoma gene. Nat. Rev. Cancer 8, 671–682.
[8] Shaw, R.J. (2009). Tumor suppression by LKB1: SIK-ness prevents metastasis. Sci. Signal. 2, pe55.
[9] Ikushima, H., and Miyazono, K. (2010). TGFbeta signalling: a complex web in cancer progression. Nat. Rev. Cancer 10, 415–424.
[10] Adams, J.M., and Cory, S. (2007). The Bcl-2 apoptotic switch in cancer development and therapy. Oncogene 26, 1324–1337.
[11] Junttila, M.R., and Evan, G.I. (2009). p53—a Jack of all trades but master of none. Nat. Rev. Cancer 9, 821–829.
[12] Grivennikov, S.I., Greten, F.R., and Karin, M. (2010). Immunity, inflammation, and cancer. Cell 140, 883–899.
[13] Blasco, M.A. (2005). Telomeres and human disease: ageing, cancer and beyond. Nat. Rev. Genet. 6, 611–622.
[14] Park, J.I., Venteicher, A.S., Hong, J.Y., Choi, J., Jun, S., Shkreli, M., Chang, W., Meng, Z., Cheung, P., Ji, H., et al. (2009). Telomerase modulates Wnt signalling by association with target gene chromatin. Nature 460, 66–72.
[15] Kawai, T., Hiroi, S., Nakanishi, K., and Meeker, A.K. (2007). Telomere length and telomerase expression in atypical adenomatous hyperplasia and small bronchioloalveolar carcinoma of the lung. Am. J. Clin. Pathol. 127, 254–262.
[16] Hanahan, D., and Folkman, J. (1996). Patterns and emerging mechanisms of the angiogenic switch during tumorigenesis. Cell 86, 353–364.
[17] Baeriswyl, V., and Christofori, G. (2009). The angiogenic switch in carcinogenesis. Semin. Cancer Biol. 19, 329–337.
[18] Ferrara, N. (2009). Vascular endothelial growth factor. Arterioscler. Thromb. Vasc. Biol. 29, 789–791.
[19] Nagy, J.A., Chang, S.H., Shih, S.C., Dvorak, A.M., and Dvorak, H.F. (2010). Heterogeneity of the tumor vasculature. Semin. Thromb. Hemost. 36, 321–331.
[20] Taddei, M. L., Giannoni, E., Fiaschi, T., & Chiarugi, P. (2012). Anoikis: an emerging hallmark in health and diseases. The Journal of pathology, 226(2), 380-393.
[21] Kalluri R, Weinberg RA. The basics of epithelial-mesenchymal transition. The Journal of Clinical Investigation. 2009;119(6):1420-1428. doi:10.1172/JCI39104.
[22] Yan C, Grimm WA, Garner WL, et al. Epithelial to Mesenchymal Transition in Human Skin Wound Healing Is Induced by Tumor Necrosis Factor-α through Bone Morphogenic Protein-2. The American Journal of Pathology. 2010;176(5):2247-2258. doi:10.2353/ajpath.2010.090048.
[23] Nieto, M. A., Huang, R. Y. J., Jackson, R. A., & Thiery, J. P. (2016). EMT: 2016. Cell, 166(1), 21-45.
[24] Karnoub, A.E., Dash, A.B., Vo, A.P., Sullivan, A., Brooks, M.W., Bell, G.W., Richardson, A.L., Polyak, K., Tubo, R., and Weinberg, R.A. (2007). Mesenchymal stem cells within tumour stroma promote breast cancer metastasis. Nature 449, 557–563.
[25] Gocheva, V., Wang, H.W., Gadea, B.B., Shree, T., Hunter, K.E., Garfall, A.L., Berman, T., and Joyce, J.A. (2010). IL-4 induces cathepsin protease activity in tumor-associated macrophages to promote cancer growth and invasion. Genes Dev. 24, 241–255.
[26] Kessenbrock, K., Plaks, V., and Werb, Z. (2010). Matrix metalloproteinases: Regulators of the tumor microenvironment. Cell 141, 52–67.
[27] Talmadge, J.E., and Fidler, I.J. (2010). AACR centennial series: the biology of cancer metastasis: historical perspective. Cancer Res. 70, 5649–5669.
[28] Naumov, G.N., Folkman, J., Straume, O., and Akslen, L.A. (2008). Tumorvascular interactions and tumor dormancy. APMIS 116, 569–585.
[29] Kenific, C.M., Thorburn, A., and Debnath, J. (2010). Autophagy and metastasis: another double-edged sword. Curr. Opin. Cell Biol. 22, 241–245.
[30] Berdasco, M., and Esteller, M. (2010). Aberrant epigenetic landscape in cancer: How cellular identity goes awry. Dev. Cell 19, 698–711.
[31] Negrini, S., Gorgoulis, V.G., and Halazonetis, T.D. (2010). Genomic instability— an evolving hallmark of cancer. Nat. Rev. Mol. Cell Biol. 11, 220–228.
[32] Lane, D.P. (1992). Cancer. p53, guardian of the genome. Nature 358, 15–16.
[33] DeNardo, D.G., Andreu, P., and Coussens, L.M. (2010). Interactions between lymphocytes and myeloid cells regulate pro- versus anti-tumor immunity. Cancer Metastasis Rev. 29, 309–316.
[34] Jones, R.G., and Thompson, C.B. (2009). Tumor suppressors and cell metabolism: a recipe for cancer growth. Genes Dev. 23, 537–548.
[35] DeBerardinis, R.J., Lum, J.J., Hatzivassiliou, G., and Thompson, C.B. (2008). The biology of cancer: Metabolic reprogramming fuels cell growth and proliferation. Cell Metab. 7, 11–20.
[36] Semenza, G.L. (2010a). HIF-1: upstream and downstream of cancer metabolism. Curr. Opin. Genet. Dev. 20, 51–56.
[37] Kennedy, K.M., and Dewhirst, M.W. (2010). Tumor metabolism of lactate: the influence and therapeutic potential for MCT and CD147 regulation. Future Oncol. 6, 127–148.
[38] Page` s, F., Galon, J., Dieu-Nosjean, M.C., Tartour, E., Saute` s-Fridman, C., and Fridman, W.H. (2010). Immune infiltration in human tumors: a prognostic factor that should not be ignored. Oncogene 29, 1093–1102.
[39] López-Otín, C., Blasco, M. A., Partridge, L., Serrano, M., & Kroemer, G. (2013). The hallmarks of aging. Cell, 153(6), 1194-1217.
[40] Foster, A. D., Sivarapatna, A., & Gress, R. E. (2011). The aging immune system and its relationship with cancer. Aging health, 7(5), 707-718.
[41] DeGregori, J. (2013). Challenging the axiom: does the occurrence of oncogenic mutations truly limit cancer development with age?. Oncogene, 32(15), 1869.
[42] Afroze Alam, U Farooq, Ruchi Singh, VP Dubey, Shailendra Kumar, et al. Chemotherapy Treatment and Strategy Schemes: A 002 Review. Open Acc J of Toxicol. 2018;2(5): 555600.
[43] Conklin KA (2000) Dietary antioxidants during cancer chemotherapy: impact on chemotherapeutic effectiveness and development of side effects. Nutr Cancer 37(1): 1-8.
[44] Baskar, R., Lee, K. A., Yeo, R., & Yeoh, K. W. (2012). Cancer and radiation therapy: current advances and future directions. International journal of medical sciences, 9(3), 193.
[45] Begg AC, Stewart FA, Vens C: Strategies to improve radio-therapy with targeted drugs. Nat Rev Cancer 2011; 11: 239-253.
[46] Barnett GC, West CM, Dunning AM, Elliott RM, Coles CE, Pharoah PD, Burnet NG: Normal tissue reactions to radiother-apy: towards tailoring treatment dose by genotype. Nat Rev Cancer 2009; 9: 134-142.
[47] Nassar, D. & Blanpain, C. Cancer stem cells: basic concepts and therapeutic implications. Annu. Rev. Pathol. 11, 47–76 (2016).
[48] Batlle, E., & Clevers, H. (2017). Cancer stem cells revisited. Nature medicine, 23(10), 1124.
[49] Harris, W.J. et al. The histone demethylase KDM1A sustains the oncogenic potential
of MLL-AF9 leukemia stem cells. Cancer Cell 21, 473–487 (2012).
[50] Gong, X. et al. LGR5-targeted antibody-drug conjugate eradicates gastrointestinal
tumors and prevents recurrence. Mol. Cancer Ther. 15, 1580–1590 (2016).
[51] Ribas, A., & Wolchok, J. D. (2018). Cancer immunotherapy using checkpoint blockade. Science, 359(6382), 1350-1355.
[52] Y. Ishida, Y. Agata, K. Shibahara, T. Honjo, EMBO J. 11,
3887–3895 (1992).
[53] C. A. Chambers, M. S. Kuhns, J. G. Egen, J. P. Allison, Annu. Rev. Immunol. 19, 565–594 (2001).
[54] M. A. Postow, R. Sidlow, M. D. Hellmann, N. Engl. J. Med. 378,
158–168 (2018).
[55] BMJ 2015;350:h988 doi: 10.1136/bmj.h988
[56] Kirkwood JM, Lee S, Moschos SJ, et al. Immunogenicity and antitumor effects of vaccination with peptide vaccine ±granulocyte-monocyte colony-stimulating factor and/or IFN-alpha2b in advanced metastatic melanoma: Eastern Cooperative Oncology Group Phase II Trial E1696. Clin Cancer Res 2009;15:1443-51.
[57] Palucka K, Banchereau J. Cancer immunotherapy via dendritic cells. Nat Rev Cancer 2012;12:265-77
[58] Vacchelli E, Vitale I, Eggermont A, et al. Trial watch: dendritic cell-based interventions for cancer therapy. Oncoimmunology 2013;2:e25771.
[59] Luiten RM, Kueter EW, Mooi W, et al. Immunogenicity, including vitiligo, and feasibility of vaccination with autologous GM-CSF-transduced tumor cells in metastatic melanoma patients. J Clin Oncol 2005;23:8978-91.
[60] Butterfield LH, Economou JS, Gamblin TC, et al. Alpha fetoprotein DNA prime and adenovirus boost immunization of two hepatocellular cancer patients. J Transl Med 2014;12:86.
[61] S. A. Rosenberg, N. P. Restifo, Science 348, 62–68 (2015).
[62] C. H. June, S. R. Riddell, T. N. Schumacher, Sci. Transl. Med. 7, 280ps7 (2015).
[63] F. Garrido, N. Aptsiauri, E. M. Doorduijn, A. M. Garcia Lora, T. van Hall, Curr. Opin. Immunol. 39, 44–51 (2016).
[64] June, C. H., O’Connor, R. S., Kawalekar, O. U., Ghassemi, S., & Milone, M. C. (2018). CAR T cell immunotherapy for human cancer. Science, 359(6382), 1361-1365.
[65] J. Gust et al., Cancer Discov. 7, 1404–1419 (2017).







![[Video] Eurosymposium on Healthy Ageing, Brussels, 2018 Eurosymposium on Healthy Aging](https://www.longlonglife.org/wp-content/uploads/2019/07/P1310252-218x150.jpg)






